Content from presentations and scholarly articles by Dr. Phoebe Rich
Nail psoriasis occurs in up to 80% of patients with plaque psoriasis and is more prevalent in patients with psoriatic arthritis. Nail psoriasis is far more than just a cosmetic problem. Psoriasis of the fingernails is psychologically distressing and can cause pain and functional deficits in fine motor manipulation of small objects. When toenails are involved, it can cause difficulty with ambulation. Although nail psoriasis can be extensively destructive to the nail plate, it is a non-scarring process. If treated effectively, nails with psoriasis can return to a normal or close to normal condition. Nail psoriasis takes a vast toll on patients, but with treatment quality of life can greatly increase.
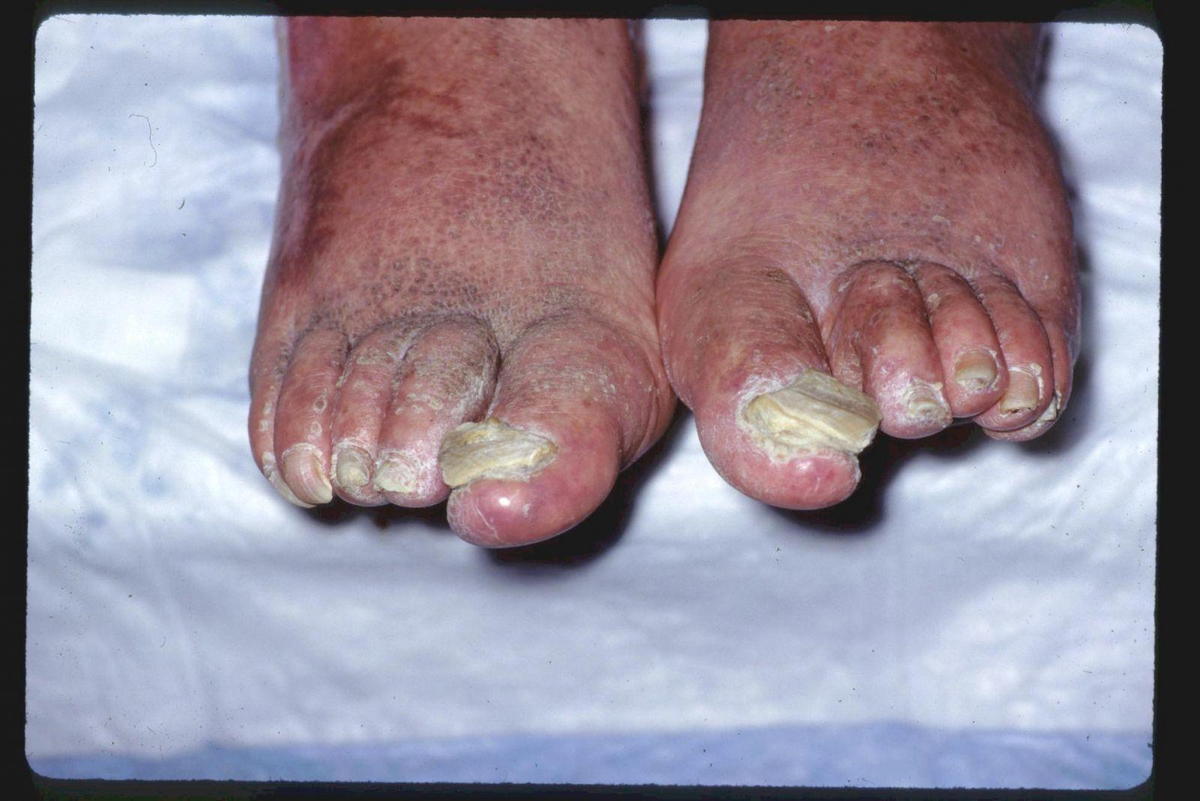
There are a few key factors by which the disease is characterized. Pitting is a common occurrence in which the keratin of the nail loses cells and forms pits in the fingernail or toenail. It can range anywhere from one pit to a dozen pits, varying from patient to patient. Oil drop discoloration is characterized by the appearance of a drop of oil under the nail-bed. It can range from yellow-red to yellow-brown in color. The nails turn white once crumbling begins to develop. If the nail starts to lift and separate from the nail bed on either the fingers or toes, this is referred to as onycholysis. Other characterizations include subungual hyperkeratosis and splinter hemorrhages.

“50% of people with Psoriasis have the disease on their nails, but only 5% have it limited to their nails.”
Nail psoriasis can also be diagnosed along with toenail fungus, Reiter’s syndrome, parakeratosis pustulosa, subungual hyperkeratosis, or fingertip eczema with subungual hyperkeratosis and onycholysis. Psoriasis can be accompanied by a secondary infection, such as yeast, fungus or dermatophytes. When fungus is involved, it can contribute to the Koebner phenomenon. Your doctor will do a KoH test or a culture on the nail and view it under the microscope for analysis.
There are many options for treating nail psoriasis. Possible options include topicals, injectable and oral medications, and physical modalities such as PUVA light therapy and Grenz Ray. Clinical features of psoriasis are isolated from the site of pathology. Challenges can arise if the nail plate prevents the delivery of medication to the the pathology. Medications are only effective when they get to where they need to go. If medications don’t work, many patients may choose to simply conceal it.
When covering up nail psoriasis it’s important to be cautious about potential Koebner reactions. If one does choose to go this route, avoid any potential allergies or irritants. While millions of women use nail cosmetics with no adverse effects to their psoriasis, cosmetic practices can cause problems in psoriatic nails just as well as non-psoriatic.
GET A SUPPORT SYSTEM!
With any disease, it’s important to have a support system. Optimism and encouragment can go a long way. Additonally, new research is being conducted at all times, as are possible trials to get involved with.
The Oregon Dermatology and Research Center is a proud supporter of the National Psoriasis Foundation. They are a great resource for individuals and families who are looking for support in the community, events, education for both adults and children alike, and ways to get involved.
